Roozehra Khan, DO, always gravitated toward critical care. As a critical care fellow at Mount Sinai Hospital in New York, she developed skills in neurocritical care and point-of-care ultrasound while working in the neuro and trauma ICU. Today, Dr. Khan is an assistant professor of clinical medicine at Keck School of Medicine of the University of Southern California and an attending critical care physician in the neurosurgical ICU.
Neurocritical care is an emerging subspecialty that began in the last 30 years. It is the intensive care management of patients with life-threatening neurological and neurosurgical illnesses.
“What I love about neurocritical care is that there’s still a lot we don’t know and it allows me to practice the art of medicine and really use my clinical judgement,” Dr. Khan says. “The brain is really interesting because it can be so resilient sometimes and other times it’s just … unforgiving.”
The DO talked with Dr. Khan recently to learn what a typical day is like for an intensivist in a neurosurgical ICU. Here’s a recap:
 6 a.m. Time to start the day!
6 a.m. Time to start the day!
7:37 a.m. Dr. Khan grabs her breakfast shake and begins her morning commute in L.A.-area traffic.
8:30 a.m. Dr. Khan arrives to work in the neurosurgical ICU at Keck.
8:30-9 a.m. Time for radiology rounds. Dr. Khan will check the CAT scans, MRIs and chest X-ray results of that day’s patients.
9 a.m.-11 a.m. or noon The whole team (consisting of an attending critical care physician, a pulmonary critical care fellow, a neurology-trained critical care physician, a neurocritical care fellow and a group of residents) will gather at the bedside of each patient, one by one. Heavier days can include about 16 patients, while most days average 10. “We’ll roll through the entire ICU,” says Dr. Khan. “The resident will present the patient and then we’ll examine the patient together and come up with an assessment and plan for the day.”
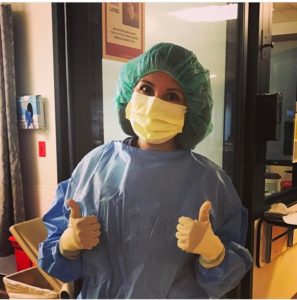 Early afternoon Time for patient procedures by the neurocritical care team. These bedside procedures can include inserting central venous catheter lines and arterial lines, endotracheal intubation, intracranial pressure monitor insertion and critical care ultrasound.
Early afternoon Time for patient procedures by the neurocritical care team. These bedside procedures can include inserting central venous catheter lines and arterial lines, endotracheal intubation, intracranial pressure monitor insertion and critical care ultrasound.
Late afternoon It’s post-op time! The neurosurgical ICU’s surgeons typically do operations in the morning, and the critical care team starts seeing neurosurgical and ENT (ear, nose and throat) post-operative patients in the afternoon. Keck will also receive transfer patients throughout the day.
“We’ll get transfers from surrounding facilities of patients who need a higher level of care. We’re a teaching hospital, so we have a lot of interventions that other hospitals don’t,” says Dr. Khan. “We have neurosurgeons that do a lot of complicated, advanced surgeries and because neurocritical care is a fairly new subspecialty, not a lot of hospitals are equipped to handle this care.”
 One of the interventions at Keck, which Dr. Khan specializes in, is point-of-care ultrasound. “This is when we (physicians) perform our own ultrasounds and interpret the images ourselves to make quick, bedside decisions,” says Dr. Khan. “We train the residents and fellows in this.”
One of the interventions at Keck, which Dr. Khan specializes in, is point-of-care ultrasound. “This is when we (physicians) perform our own ultrasounds and interpret the images ourselves to make quick, bedside decisions,” says Dr. Khan. “We train the residents and fellows in this.”
5-6 p.m. Calling it a day! It’s time to head home. “Of course, my shifts can get later if there’s someone who’s really sick.”
7 p.m. Dinner and unwinding in the girl cave, at last.
More on neurocritical care
The general critical care field is highly fulfilling, says Dr. Khan, but it can exert its toll on a physician if they take patient outcomes personally or bring the job home with them.
“Physicians who wind up gravitating toward the critical care subspecialty are usually prepared for the ups and downs of the ICU,” says Dr. Khan.
Dr. Khan’s typical patients run the gamut, from older patients who have suffered strokes to middle-age ones with subarachnoid hemorrhages to younger patients with traumatic brain injuries, as well as post-operative brain tumor patients of any age.
“I do have cases that are very rewarding where the patient has a good outcome,” says Dr. Khan, “but, of course, I’ll have those devastating cases where the patient is severely comatose or ends up brain dead.”
Keeping burnout at bay
While critical care has one of the highest burnout rates of any medical subspecialty, Dr. Khan has found ways to deal with the high stress and has even overcome her own burnout. First and foremost, she balances her emotions by engaging in a lot of self-care.
“I don’t take my patients’ bad outcomes personally, and I don’t internalize them,” says Dr. Khan, who blogs at the thefemaledoc.com. “When I’m off work, I do things that I love—like spend time with friends and family, travel, golf and write. I don’t take my work home.”
Becoming a neurocritical care physician
The neurocritical care subspecialty is neither ACGME nor AOA certified. Rather, the United Council for Neurologic Subspecialties (UCNS) administers the board exams.
UCNS will allow osteopathic physicians to sit for the boards, but only osteopathic physicians who completed their training in ACGME-accredited settings and have their primary certification through an ABMS (American Board of Medical Specialties) board, says Josh Prober, general counsel and senior vice president for the American Osteopathic Association. “The AOA’s advocacy on this matter is ongoing and UCNS is resisting change.”
Some physicians, including Dr. Khan, have found an alternate path to the subspecialty by obtaining certification in critical care and then working in a neurological ICU.
Article reposted with permission from The DO, a monthly online magazine published by the American Osteopathic Association. Subscribe to their weekly roundup emails.
+ show Comments
- Hide Comments
add a comment